Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (51): 8275-8280.doi: 10.3969/j.issn.2095-4344.2014.51.014
Previous Articles Next Articles
Expression and significance of interleukin-17 in rejection after kidney transplantation
Sun Shu1, Li Zhou-li2, Cai Ming2, Wang Qiang2, Jin Hai-long2, Chen Chang-qing2, Liu Zhi-jia2, Kong Xiang-rui2, Li Cong-ran2, Shi Bing-yi2
- 1Military Medical Science Academy of PLA, Beijing 100039, China; 2Organ Transplant Institute, the 309th Hospital of PLA, Beijing 100091, China
-
Online:2014-12-10Published:2014-12-10 -
Contact:Shi Bing-yi, Doctoral supervisor, Chief physician, Organ Transplant Institute, the 309th Hospital of PLA, Beijing 100091, China -
About author:Sun Shu, Studying for master’s degree, Military Medical Science Academy of PLA, Beijing 100039, China -
Supported by:theNational Natural Science Foundation of China, No. 81171753
CLC Number:
Cite this article
Sun Shu, Li Zhou-li, Cai Ming, Wang Qiang2 Jin Hai-long, Chen Chang-qing, Liu Zhi-jia, Kong Xiang-rui, Li Cong-ran, Shi Bing-yi. Expression and significance of interleukin-17 in rejection after kidney transplantation[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(51): 8275-8280.
share this article
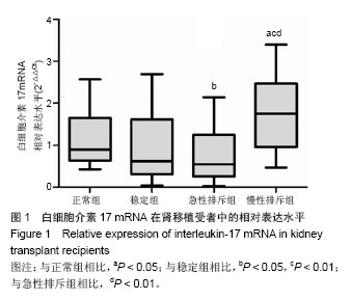
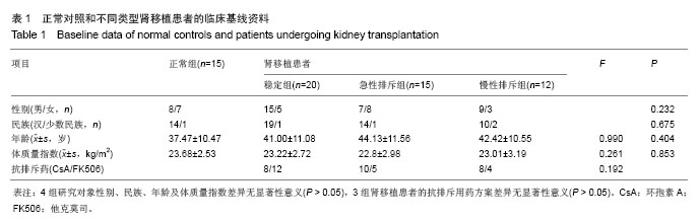
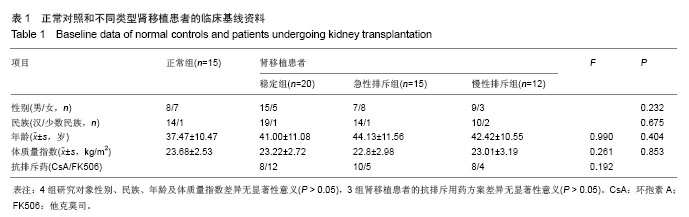
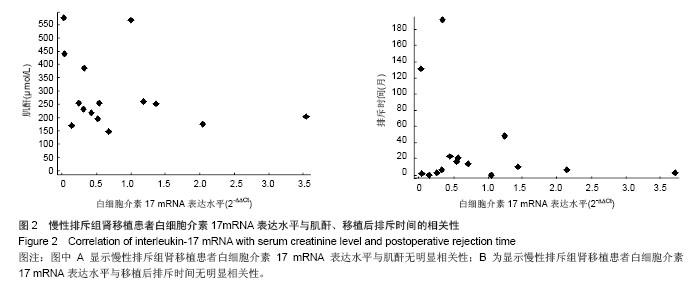
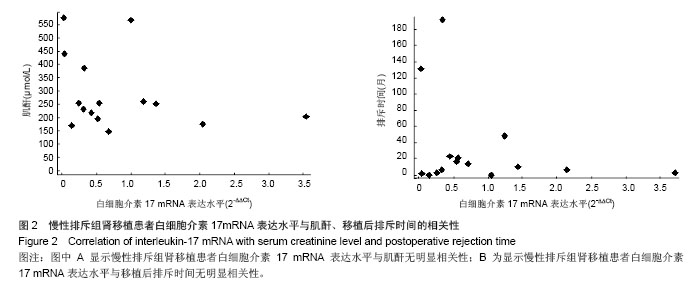
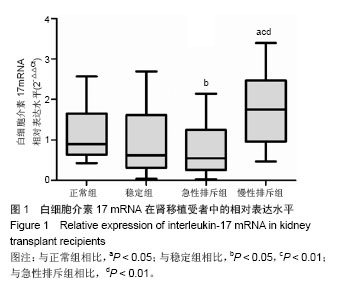
2.2 肾移植患者血清肌酐值及排斥时间 正常组、稳定组、急性排斥组和慢性排斥组对象血清肌酐值分别为(64.073±13.443),(97.620±21.592),(295.240±137.644),(258.717±78.180) μmol/L,经秩和检验统计分析,差异有显著性意义(H=50.351,P=0.000 0 < 0.05)。其中急性排斥组和慢性排斥组患者血清肌酐值差异无显著性意义(P > 0.05)。 在急性排斥组患者移植肾的排斥时间从0.75-192个月,中位排斥时间为13个月;在慢性排斥组患者移植肾的排斥时间在24-168个月,中位排斥时间为88.5个月。因2组数据不呈正态分布,故经秩和检验差异有显著性意义(P=0.004 < 0.05)。 2.3 白细胞介素17 mRNA在肾移植受者中的相对表达 与正常组相比,急性排斥组与稳定组患者白细胞介素17 mRNA的表达水平差异有显著性意义;而慢性排斥组患者白细胞介素17 mRNA较稳定组升高了2.89倍(P < 0.01;图1)。"
| [1]Thaunat O, Legendre C, Morelon E, et al. To biopsy or not to biopsy? Should we screen the histology of stable renal grafts? Transplantation. 2007;84(6):671-676. [2]Omasa M, Fukuse T, Toyokuni S, et al. Glycine ameliorates lung reperfusion injury after cold preservation in an ex vivo rat lung model. Transplantation. 2003;75(5):591-598. [3]Serody JS, Hill GR. The IL-17 differentiation pathway and its role in transplant outcome. Biol Blood Marrow Transplant. 2012; 18(1 Suppl):S56-61. [4]Steinman L. A brief history of T(H)17, the first major revision in the T(H)1/T(H)2 hypothesis of T cell-mediated tissue damage. Nat Med. 2007;13(2):139-145. [5]Laurence A, Tato CM, Davidson TS, et al. Interleukin-2 signaling via STAT5 constrains T helper 17 cell generation. Immunity. 2007;26(3):371-381. [6]Veldhoen M, Hocking RJ, Atkins CJ, et al. TGFbeta in the context of an inflammatory cytokine milieu supports de novo differentiation of IL-17-producing T cells. Immunity. 2006; 24(2):179-189. [7]Louten J, Boniface K, de Waal Malefyt R. Development and function of TH17 cells in health and disease. J Allergy Clin Immunol. 2009;123(5):1004-1011. [8]Sonnenberg GF, Weiner DB. Manipulation of T(H)17 responses in pulmonary immunity and disease through vaccination. Hum Vaccin. 2009;5(8):510-519. [9]Goriely S, Cavoy R, Goldman M. Interleukin-12 family members and type I interferons in Th17-mediated inflammatory disorders. Allergy. 2009;64(5):702-709. [10]Fouser LA, Wright JF, Dunussi-Joannopoulos K, et al. Th17 cytokines and their emerging roles in inflammation and autoimmunity. Immunol Rev. 2008;226:87-102. [11]Cua DJ, Tato CM. Innate IL-17-producing cells: the sentinels of the immune system. Nat Rev Immunol. 2010;10(7): 479-489. [12]Iwakura Y, Nakae S, Saijo S, et al. The roles of IL-17A in inflammatory immune responses and host defense against pathogens. Immunol Rev. 2008;226:57-79. [13]Annunziato F, Cosmi L, Liotta F, et al. The phenotype of human Th17 cells and their precursors, the cytokines that mediate their differentiation and the role of Th17 cells in inflammation. Int Immunol. 2008;20(11):1361-1368. [14]Peters A, Lee Y, Kuchroo VK. The many faces of Th17 cells. Curr Opin Immunol. 2011;23(6):702-706. [15]Szabo SJ, Sullivan BM, Stemmann C, et al. Distinct effects of T-bet in TH1 lineage commitment and IFN-gamma production in CD4 and CD8 T cells. Science. 2002;295(5553):338-342. [16]Kolls JK, Lindén A. Interleukin-17 family members and inflammation. Immunity. 2004;21(4):467-476. [17]Li T, Si Z, Qi H, et al. IL-17 in the early diagnosis of acute renal allograft rejection in mice. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2011;36(12):1147-1152. [18]Xie XJ, Ye YF, Zhou L, et al. Th17 promotes acute rejection following liver transplantation in rats. J Zhejiang Univ Sci B. 2010;11(11):819-827. [19]Vanaudenaerde BM, Dupont LJ, Wuyts WA, et al. The role of interleukin-17 during acute rejection after lung transplantation. Eur Respir J. 2006;27(4):779-787. [20]熊俊杰,陆慧敏,杜晓炯,等.Th17细胞在胰岛移植中的作用[J].四川大学学报(医学版),2010,41(4):638-643. [21]Li J, Simeoni E, Fleury S, et al. Gene transfer of soluble interleukin-17 receptor prolongs cardiac allograft survival in a rat model. Eur J Cardiothorac Surg. 2006;29(5):779-783. [22]Yapici Ü, Kers J, Bemelman FJ, et al. Interleukin-17 positive cells accumulate in renal allografts during acute rejection and are independent predictors of worse graft outcome. Transpl Int. 2011;24(10):1008-1017. [23]de Boer OJ, van der Meer JJ, Teeling P, et al. Differential expression of interleukin-17 family cytokines in intact and complicated human atherosclerotic plaques. J Pathol. 2010; 220(4):499-508. [24]Parrish-Novak J, Dillon SR, Nelson A, et al. Interleukin 21 and its receptor are involved in NK cell expansion and regulation of lymphocyte function. Nature. 2000;408(6808):57-63. [25]Mehta DS, Wurster AL, Grusby MJ. Biology of IL-21 and the IL-21 receptor. Immunol Rev. 2004;202:84-95. [26]Spolski R, Leonard WJ. Interleukin-21: basic biology and implications for cancer and autoimmunity. Annu Rev Immunol. 2008;26:57-79. [27]Vassalli G, Fleury S, Li J, Goy JJ, et al. Gene transfer of cytoprotective and immunomodulatory molecules for prevention of cardiac allograft rejection. Eur J Cardiothorac Surg. 2003;24(5):794-806. [28]Lubberts E. IL-17/Th17 targeting: on the road to prevent chronic destructive arthritis? Cytokine. 2008;41(2):84-91. Butcher M, Galkina E. Current views on the functions of interleukin-17A-producing cells in atherosclerosis. Thromb Haemost. 2011;106(5):787-795. [29]Pappu R, Ramirez-Carrozzi V, Sambandam A. The interleukin-17 cytokine family: critical players in host defence and inflammatory diseases. Immunology. 2011;134(1):8-16. [30]Shi J, Li Y, Yang X, et al. Upregulation of α-enolase in acute rejection of cardiac transplant in rat model: implications for the secretion of interleukin-17. Pediatr Transplant. 2014;18(6): 575-585. [31]Winton HL, Bidwell JL, Armitage WJ. Haplotype analysis on chromosome 6p of tumor necrosis factor alpha, vascular endothelial growth factor A, and interleukin-17F alleles associated with corneal transplant rejection. Transplant Proc. 2014;46(5):1540-1547. [32]Xu Q, Zheng F, Gong F, et al. Suppressor of cytokine signaling 3 (SOCS3) gene transfer prolongs the survival of the murine cardiac allograft by attenuating interleukin-17- producing alloreactive T-cell responses. J Gene Med. 2014; 16(3-4):66-74. [33]Shi X, Zhang M, Liu F, et al. Tim-1-Fc suppresses chronic cardiac allograft rejection and vasculopathy by reducing IL-17 production. Int J Clin Exp Pathol. 2014;7(2):509-520. [34]Karimi MH, Hejr S, Geramizadeh B, et al. Study of the relationships between IL-23R, IL-17, IL-21 polymorphisms and serum level of IL-17, IL-21 with acute graft rejection in iranian liver transplant recipients. Immunol Invest. 2014; 43(1):69-85. [35]Lemaître PH, Vokaer B, Charbonnier LM, et al. IL-17A mediates early post-transplant lesions after heterotopic trachea allotransplantation in Mice. PLoS One. 2013;8(7): e70236. [36]Parrish-Novak J, Dillon SR, Nelson A, et al. Interleukin 21 and its receptor are involved in NK cell expansion and regulation of lymphocyte function. Nature. 2000;408(6808):57-63. [37]Coquet JM, Kyparissoudis K, Pellicci DG, et al. IL-21 is produced by NKT cells and modulates NKT cell activation and cytokine production. J Immunol. 2007;178(5):2827-2834. [38]王小飞,张轶,张玉君,等.IL-17及IL-22在大鼠肝移植排斥反应中的表达及意义[J].免疫学杂志,2012,28(5):369-373. [39]Dolff S, Abdulahad WH, Westra J, et al. Increase in IL-21 producing T-cells in patients with systemic lupus erythematosus. Arthritis Res Ther. 2011;13(5):R157. [40]Zhu C, Ma J, Liu Y, et al. Increased frequency of follicular helper T cells in patients with autoimmune thyroid disease. J Clin Endocrinol Metab. 2012;97(3):943-950. [41]杜国盛,郑慧丽,石炳毅,等.IL-17在小鼠皮肤移植受者外周血及移植物中的表达[J].解放军医学杂志,2009,34(11):1285-1287. [42]Balázs C. The role of hereditary and environmental factors in autoimmune thyroid diseases. Orv Hetil. 2012;153(26): 1013-1022. [43]Lepez T, Vandewoestyne M, Deforce D. Fetal microchimeric cells in autoimmune thyroid diseases: harmful, beneficial or innocent for the thyroid gland? Chimerism. 2013;4(4):111-118. [44]Martin A, Davies TF. T cells and human autoimmune thyroid disease: emerging data show lack of need to invoke suppressor T cell problems. Thyroid. 1992;2(3):247-261. [45]Patakas A, Platt AM, Butcher JP, et al. Putative existence of reciprocal dialogue between Tfh and B cells and its impact on infectious and autoimmune disease. Immunol Lett. 2011; 138(1): 38-46. [46]Tsai LM, Yu D. Follicular helper T-cell memory: establishing new frontiers during antibody response. Immunol Cell Biol. 2014;92(1):57-63. [47]Ahearne MJ, Allchin RL, Fox CP, et al. Follicular helper T-cells: expanding roles in T-cell lymphoma and targets for treatment. Br J Haematol. 2014;166(3):326-335. [48]Sutherland AP, Van Belle T, Wurster AL, et al. Interleukin-21 is required for the development of type 1 diabetes in NOD mice. Diabetes. 2009;58(5):1144-1155. [49]Li XY, Wu ZB, Ding J, et al. Role of the frequency of blood CD4(+) CXCR5(+) CCR6(+) T cells in autoimmunity in patients with Sjögren's syndrome. Biochem Biophys Res Commun. 2012;422(2):238-244. [50]Manzo A, Vitolo B, Humby F, et al. Mature antigen- experienced T helper cells synthesize and secrete the B cell chemoattractant CXCL13 in the inflammatory environment of the rheumatoid joint. Arthritis Rheum. 2008;58(11):3377- 3387. [51]McGuire HM, Walters S, Vogelzang A, et al. Interleukin-21 is critically required in autoimmune and allogeneic responses to islet tissue in murine models. Diabetes. 2011;60(3):867-875. [52]杨一芬,陈远林,杨静芬.CD4+CD25+Foxp3+Treg调节性T细胞与移植肾长期存活的关系[J].广东医学,2011,32(1):66-69. [53]Meguro A, Ozaki K, Oh I, et al. IL-21 is critical for GVHD in a mouse model. Bone Marrow Transplant. 2010;45(4):723-729. |
| [1] | Wang Xiaobo, Wang Changan, Han Jianle, Yang Qingyan, Yang Shuaiping, Yang Junwei. Influence of conversion from cyclosporine to tacrolimus on glucose metabolism and cardiovascular risk profiles in stable kidney transplant patients [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2236-2240. |
| [2] | Liu Junchang, Gao Xiaolin, Jiang Taimao. Correlation of CY3A5 genetic polymorphism with concentration/dosage of tacrolimus and individualized administration of tacrolimus after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1740-1744. |
| [3] | Guo Juan, Zheng Shan, Xie Hui, Hu Yahui. An analysis of pathogenic bacteria infection in 422 kidney transplant recipients [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(32): 5198-5202. |
| [4] | Liu Luhao, Fang Jiali, Zhang Lei, Li Guanghui, Xu Lu, Lai Xingqiang, Xiong Yunyi, Chen Rongxin, Ma Junjie, Chen Zheng. Clinical assessment criteria of donor pancreas transplants for simultaneous pancreas-kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4157-4161. |
| [5] | Feng Yang, Yan Xu, Wang Yongkui, Yang Tengyue, Shang Lijie, Zhang Chunlin. Relationship between degenerative lumbar disc disease and peripheral blood lymphocyte subsets [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(17): 2630-2635. |
| [6] | Liu Ting, Yang Tingting, Ma Xiaona, Ma Haibin, Jin Yiran, Liang Xueyun. Immunoregulation of allograft rejection: a role played by human CD200+ sub-population from human placenta-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(13): 2068-2073. |
| [7] | Zhao Xiao1, Zhang Fengbo2, Wang Hongying1, Yan Fang3, An Mengting1, Li Yujiao1, Pang Nannan4, Ding Jianbing1. Dominant T cell and B cell epitopes in EgA31 protein of Echinococcus granulosus by bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(7): 1078-1083. |
| [8] | Yang Jin, Zhang Meixia, Yan Pei, Cheng Qiao, Li Jianzhen . Meta-analysis of risk factors for new-onset diabetes mellitus after kidney transplantation [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(15): 2450-2460. |
| [9] | Xu Xiaoling, Pan Wangping, Lü Xiaojun, Zhang Ju, Hu Yuanhua, He Kaiyong. Immunotoxicity of absorbable silk fibroin biofilm on rats [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2190-2195. |
| [10] | Li Weiwei, Li Xiaofeng, Hou Ping, Li Jianping. CD4+T and Treg immunomodulatory functions after culture with the supernatant of human placenta mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(1): 85-89. |
| [11] | Yang Qi-shun1, Jiang Wei1, Huang Chi-bing2. Staging diagnosis and treatment for pulmonary infection after renal transplantation can improve the stability of transplanted renal functions [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(8): 1255-1260. |
| [12] | Wang Jin, Niu Ben, Ma Xiao-rong, Zhang Wang-gang. Effects of recombinant human granulocyte colony-stimulating factor on CXC chemokine receptor 4 expression and chemotaxis in bone marrow microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(33): 5268-5273. |
| [13] | Niu Zi-han1, Ran Xin-jian2, Mawlan•Mamut1, Pan Chuan-peng1, He Dong-hang3, Ren Cong-gai3, Xu Qi4. Changes of microenvironment in a rat model of arthritis treated by the combination of methotrexate and diclofenac sodium [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(32): 5163-5168. |
| [14] | Li Ling1, Xu Qian1, Wei Wan-hui1, Zhao Hui-jia1, Shi Yu-ying1, Liu Lu1, Wang Yan-feng1, Ye Qi-fa1, 2 . Lung injury and inflammatory responses in a rabbit model of brain death [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(28): 4481-4486. |
| [15] | Gong Yu-bo1, Liu Yong2, Zhao Hong-wei1, Xu Qian-qian1, Guo Hui-ling1 . Expression levels of Foxp3 and indoleamine 2,3-dioxygenase in mouse corneal allograft rejection [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(28): 4513-4517. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||